When you’re literally not feeling well, it may be time to get your muscles and nerves tested.
Indications for Electrodiagnostic Testing
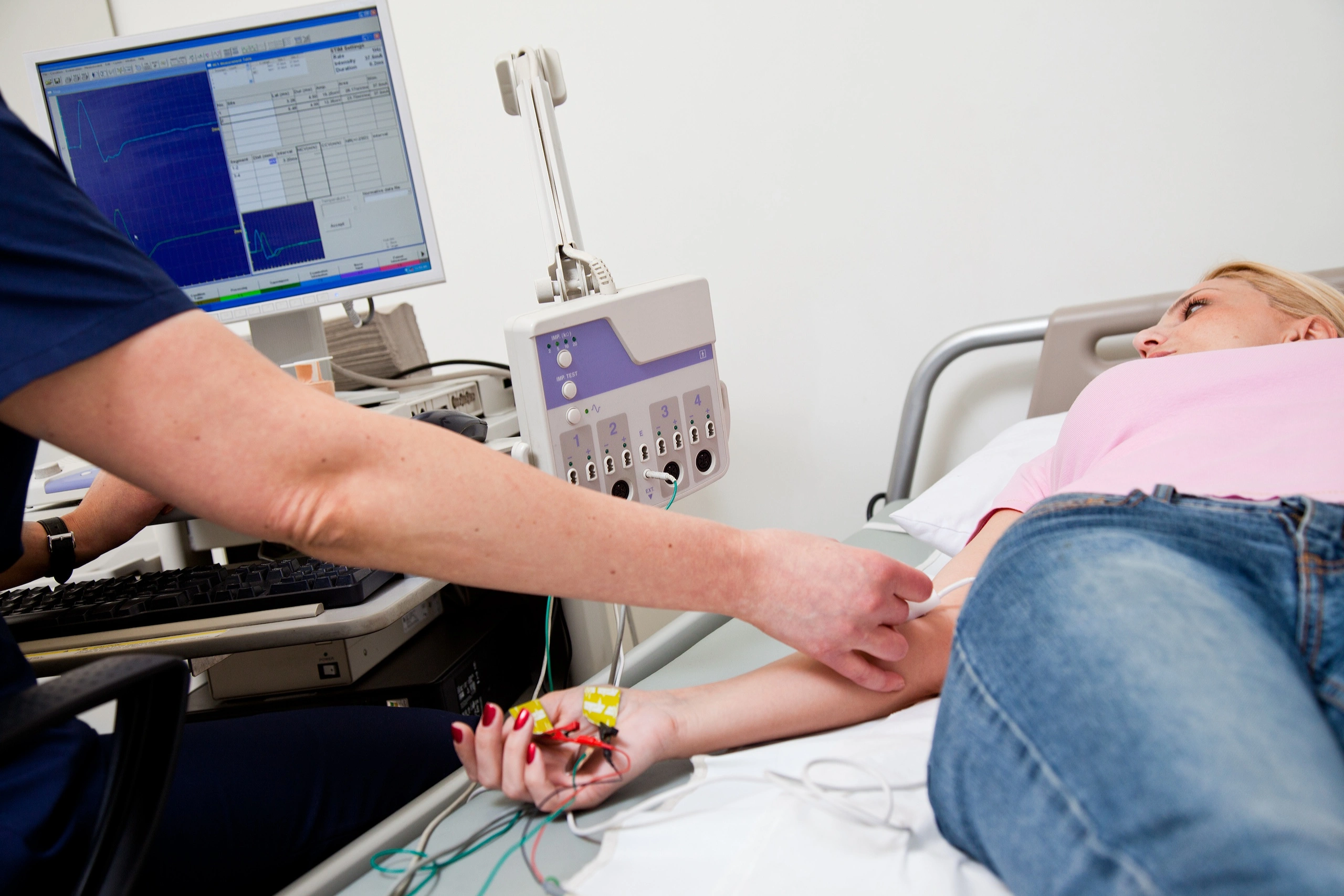
Specialized testing of the muscles and nerves called electrodiagnostic testing (EDX) is commonly performed at Mountain Medical Practice to evaluate symptoms associated with a gamut of conditions ranging from minor nerve irritations to serious neuromuscular diseases. Testing is performed using a machine that detects and measures electrical impulses transmitted through the body. Symptoms investigated often include alterations in skin sensation, muscle weakness, problems with coordination, difficulty walking, or a painful neck or back.
Sensory Disturbances
You may “…feel those needles and pins…hurtin’…hurtin’…” *
* “Needles and Pins” is a song written by Sonny Bono and Jack Nitzsche released by Jackie DeShannon 04/11/1963 and The Searchers 01/07/1964.

Abnormal skin sensations may feel like pins and needles, numbness, tingling, burning, or electric sensations. It may become difficult to sense hot and cold temperatures, or difficult to discriminate between objects of different textures.
The conditions that may be detected with electrodiagnostic testing span a broad range, from irritated, injured, or overused nerves as in Carpal Tunnel Syndrome, to various types of muscular dystrophies, Bell’s Palsy, Guillain-Barré Syndrome, Myasthenia Gravis, and Lou Gehrig’s Disease, to name a few. Nerve conduction studies can detect neuropathies in which nerve fibers in the toes and hands become injured or dysfunctional often due to uncontrolled diabetes, too much alcohol, Vitamin B12 deficiency, infections like Lyme disease, inherited disorders, chemotherapy side effects, or exposure to toxic substances, such as lead.
Paresthesias & Dysesthesias
Paresthesias are abnormal sensations, usually unpleasant, such as numbness, itching, or tickling, that occur spontaneously without a specific stimulus, often in the arms, hands, legs, or feet.
Dysesthesias are abnormal sensations that may be more irritating or painful, such as stinging, prickling, stabbing, burning, or zapping in the limbs
Patients suffering from paresthesias or dysesthesias may say, “My feet are on fire!” or “It feels like ants are crawling on my legs!”

Patients with a severe peripheral neuropathy may not feel the ground under their feet and can sometimes unknowingly burn their feet when walking over hot sand on the beach.
The decision to perform EDX testing is determined based on a patient’s symptoms, physical examination findings, and results of other diagnostic testing when appropriate, such as radiological imaging and clinical laboratory tests. Further exploration with EDX testing is usually prompted by physical exam findings of numbness in a particular pattern in the hands, arms, feet, or legs; a weak, drooping or dragging foot; a wrist drop; a loss of reflexes; or shooting pain brought on by lifting the leg or turning the neck. Persistent symptoms even in absence of abnormal exam findings may also prompt EDX testing in order to elucidate subtle neurological abnormalities and point to the source of the problem, which might otherwise go undetected. EDX testing can be thought of as an extension of the neurological physical examination and may provide greater sensitivity and accuracy in arriving at a clinical diagnosis.
Think you need an EMG test?
Sciatica and Radiculopathy
Painful sensations in the neck and back may be due to an underlying nerve root irritation. A spinal nerve root in the neck or back may become irritated by a bulging disc or an arthritic bone spur that compresses the nerve and narrows its pathway in the bony spinal canal. Pain may radiate or shoot down the arms or legs. Pain may become aggravated with certain movements, such as bending forward, lifting the arms overhead, stretching the thighs, or turning the neck. Pain may be aggravated with coughing or sneezing.

A pain in the butt…
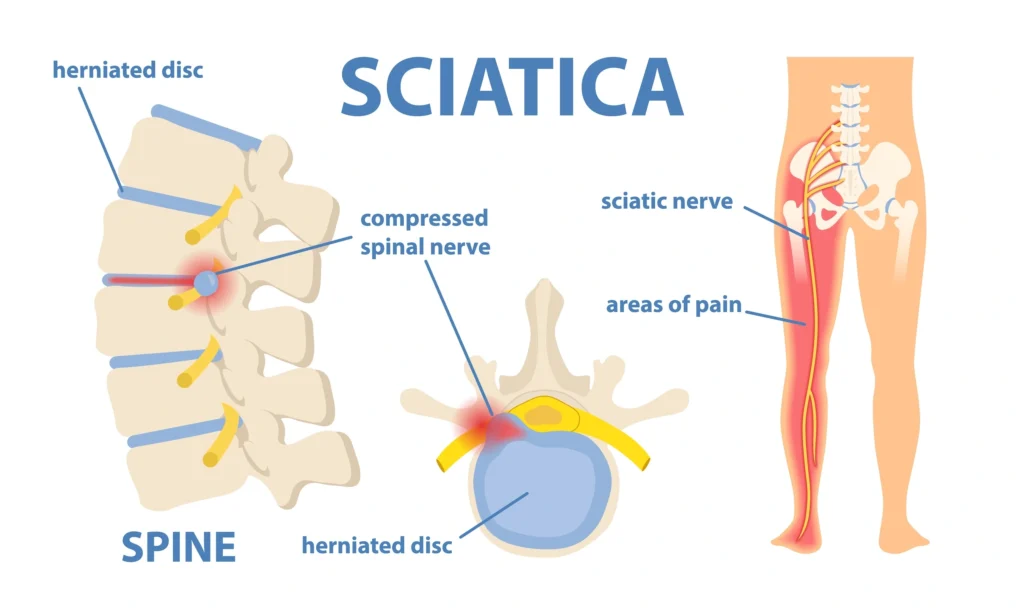
Sciatica is nerve pain from injury or irritation of the sciatic nerve. The sciatic nerve is a large nerve that travels through the buttocks down the back of the thigh and leg to the foot. It is the longest nerve in the human body. The sciatic nerve and its sensory nerve branches provide sensation to the skin of the buttocks, the back of the thigh, the back and the outer side of the lower leg, and the foot. The sciatic nerve and its motor nerve branches control the muscles that move the hip, knee, ankle and foot.
Radiculopathy is a condition in which nerve roots exiting the lower spinal canal are compressed, pinched, inflamed, or irritated. Radicular pain typically radiates from the lower back through the buttocks and can advance past the thighs into the legs and feet. Radicular pain may occur in various patterns involving one or both lower limbs depending on the particular nerve root(s) affected, and it may follow the path of the sciatic nerve or that of other nerves.
Muscle Control and Coordination
Muscular symptoms may include cramps, spasms, frequent muscle twitches, muscle weakness, muscle thinning or loss of muscle bulk. Other concerning symptoms that warrant investigation may involve lack of coordination of the hands or feet, balance problems, difficulty walking, frequent falls, and loss of control of bladder or bowel function.
Are you “overreaching”?
One may find it difficult to hold or grasp objects in hand and notice oneself dropping objects more frequently.
Oops…

About the Electrodiagnostic Test Procedure
The EDX test procedure is relatively simple. It can be performed in the office and usually takes anywhere from 15 minutes to an hour depending on the number of nerves tested. There are two parts to the test, nerve conduction studies (NCS) and electromyography (EMG), usually performed together during the same session. The test is usually performed with the patient resting in a reclining position on a comfortable examination table so that the muscles being tested are relaxed.
Nerve Conduction Studies (NCS)
NCS are usually performed first.
NCS are designed to test the functioning of peripheral nerves that transmit electrical impulses through the arms and legs. Small electrode sensors capable of transmitting and recording electric signals will be secured to the skin on one end and connected by an insulated wire to the testing machine on the other end. A low-grade electric stimulation (a very small, harmless, electric shock) is applied in order to stimulate nerves and to provoke a measurable electric response. You may feel a mild, transient, tingling sensation and you may see your muscle twitch or jerk for a moment. This is normal to experience.
Nerve responses are visible as waveforms on a computer screen monitor.
Nerve response time or latency is the time it takes in milliseconds for the stimulator to provoke a nerve response in the body, basically showing how fast your body responds to a small electric shock. Nerve conduction speed or velocity is a calculation of how fast in meters per second an electrical impulse travels through a nerve across a particular measured segment of the arm or leg. Nerve response strength depends on the number of nerve fibers that are activated and firing at the same time and is measured in millivolts of height or amplitude of a waveform.
Results are compared with standardized normal values matched for age and height and for symmetry with the opposite limb. Abnormal values, such as prolonged response times, slowed nerve conduction speeds, or weak, low-amplitude responses may indicate damage to the peripheral nerves, either by harm to the outer myelin sheath that insulates the nerve, or by harm to the inner axon fibers that transmit nerve impulses, or both.

Any abnormalities detected will be interpreted in correlation with the patient’s clinical presentation and known risk factors to determine the cause.
Electromyography (EMG)
EMG is usually performed second, after NCS are completed.
The EMG electrode sensor is compacted into two fine wires inside a thin, flexible needle that gets inserted through the skin into the underlying muscle. The needle is designed to glide easily into the target muscle causing minimal discomfort to the patient. The needle electrode broadcasts electrical activity from the muscle that can be detected both by visual waveforms on a computer monitor and by audio input through an amplifier that usually sounds like static or popping noises.
Look and listen to a live EMG recording here.
The examiner may select a group of muscles for testing, usually 5 or more muscles from each limb on the average. The muscles are first tested while at rest when they are expected to be electrically quiet in the sense that there is little to no noise heard, and the waveform display shows a relative flat line appearance. Abnormal spontaneous electric activity observed while a muscle is at rest is usually an indicator of denervation, reflecting that there has been some type of damage to the nerve controlling the muscle.
The examiner may then ask the patient to voluntarily contract the muscle against resistance, as in flexing an elbow (contracting the biceps muscle) or extending a knee (contracting the quadriceps muscle). Abnormal recruitment of muscle fibers may indicate a problem with either the muscles or the nerves.
After the Electrodiagnostic Test
The examiner will usually review and interpret your test results and discuss clinical impressions and conclusions with you before the test session is through. The test results will often provide valuable and contributory information towards your diagnosis and treatment plan.
Have questions about EMG testing? Find quick answers here.
Manual Tasks
Manual dexterity is a key factor necessary for many functional daily tasks. A change in hand grip or coordination can sometimes be an early warning sign of a muscle or nerve disorder. One may feel clumsy or start to fumble while handling objects, particularly when overtired. Symptom onset may be subtle, insidious, and slow.
Pain may be provoked with repetitive keyboard typing, knitting, crocheting, sewing, dishwashing, driving, or while holding a book or tablet.

A deterioration in handwriting can be a harbinger of various medical conditions, such as essential tremor, Parkinson’s disease, a stroke, or even arthritis. More commonly, handwriting changes may be associated with carpal tunnel syndrome, age, stress, fatigue, or mood.
Carpentry projects, wielding tools, carving, gardening, cooking, and other chores may be affected.
Don’t get discouraged!

The first step toward “fixing” things is to find out where the problem lies.
Uses for EMG and Nerve Conduction Studies
Electrodiagnostic (EDX) testing is often used to localize nerve lesions.
EDX testing may be correlated with spine imaging, such as an MRI scan. When an MRI shows a displaced bulging disc compressing a nerve root, EDX testing can determine if the irritated nerve root has become damaged or dysfunctional or if the nerve remains functionally unaffected. EDX testing can also determine severity and prognosis for recovery.
EDX testing can be helpful in guiding spinal surgical decisions as in lumbar discectomy to decrease sciatic pain or to prevent leg weakness. EDX testing may also determine if criteria are met for carpal tunnel release surgery to reduce tingling and weakness in the wrist and hand or ulnar nerve transposition surgery to relieve a painful, sensitive elbow. Serial EDX testing can also serve to assess and monitor functional recovery of the muscles and nerves, sometimes used after surgery has been performed, other times used in hopes of avoiding a surgical intervention.
Nerve & Muscle Conditions
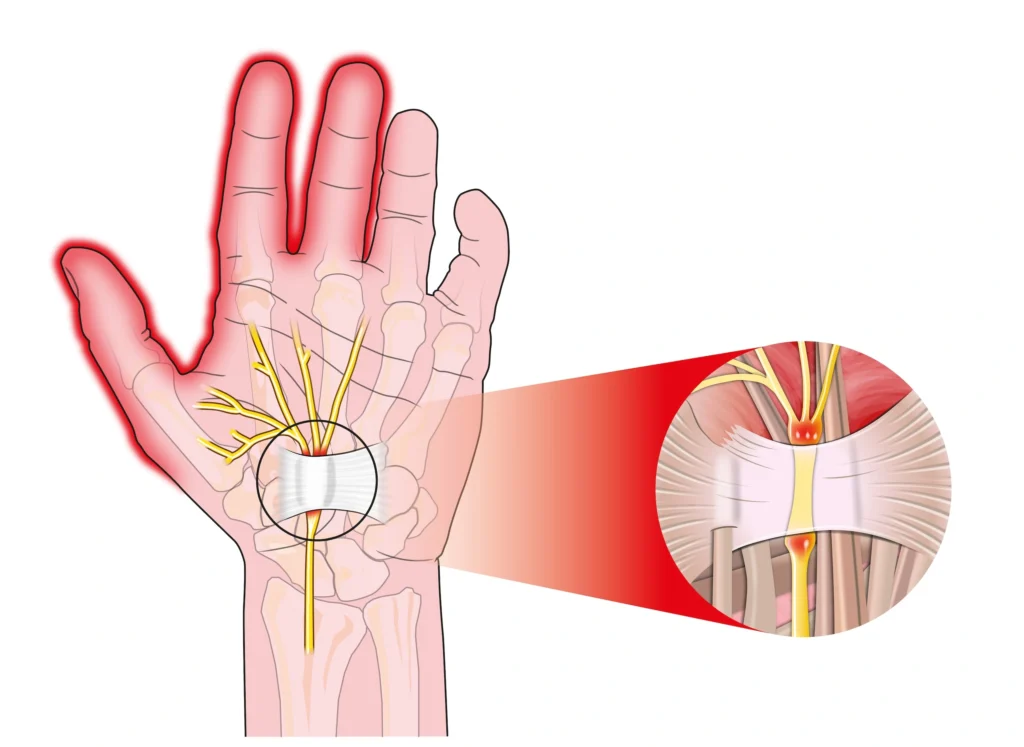
Carpal Tunnel Syndrome (CTS), a condition in which the median nerve becomes compressed at the wrist, is commonly detected with EDX testing.
EDX testing is also useful in diagnosing the following neuromuscular conditions (as well as many others not listed here).
- Cervical Radiculopathy (Pinched nerve in neck)
- Lumbar Radiculopathy (Pinched nerve in low back)
- Cubital Tunnel Syndrome (Ulnar nerve entrapped at elbow)
- Tarsal Tunnel Syndrome (Tibial nerve entrapped at ankle)
- Peroneal Neuropathy at Fibula (Nerve compressed at the outer knee)
- Piriformis Syndrome (Sciatic nerve irritated by piriformis muscle)
- Saturday Night Palsy (Radial nerve pressure at upper arm often causing wrist drop)
- Peripheral Polyneuropathy (Diabetic, Alcoholic, Toxic, Hereditary, Infectious, Idiopathic, Other)
- Chronic Inflammatory Demyelinating Polyneuropathy (CIDP)
- Diabetic Amyotrophy (Affects nerves to the hip, thigh, and buttocks)
- Bell’s Palsy
- Guillain Barré Syndrome (GBS)
- Thoracic Outlet Syndrome (TOS)
- Brachial Plexopathy
- Lumbar Plexopathy
- Myopathy
- Muscular Dystrophy
- Myasthenia Gravis
- Eaton-Lambert Syndrome
- Mononeuritis Multiplex
- Neuromyotonia
- Amyotrophic Lateral Sclerosis (ALS or Lou Gehrig’s Disease)
- Post-Polio Syndrome (Late effects Poliomyelitis)
- Charcot-Marie-Tooth Disease (Inherited neuropathy)
See other conditions treated at Mountain Medical Practice.
History of Electrodiagnostic Testing
Electrodiagnostic theory originated in the 1600’s when scientists started to experiment with electricity and muscle contraction, including Francesco Redi working with the electric eel. By the late 1700’s, Luigi Galvani (credited as the Father of Electrophysiology) used electric stimulation to make frog legs dance.

By the mid 1800’s, somewhat after the first electric battery was invented by Alessandro Volta, the first human EMG test was performed using a primitive technique to record electric activity from muscle movements of the hands. Large advances in the use of EMG for diagnostic and biomechanical applications occurred a century later throughout the 1950’s, 1960’s and 1970’s, such that by the 1980’s EMG machines were mass produced. The early EMG machine models used to electrically stimulate muscles served as precursors to both our modern EMG machine and to the TENS unit, a therapeutic device used commonly in many physical rehabilitation programs today.
In addition to EMG use as a diagnostic tool for assessing low back pain and identifying neuromuscular diseases, EMG signals are being used more broadly in a variety of applications, including the analysis of abnormal human walking patterns, improved performance in sports, forensic analysis of facial muscles to determine emotions and motivation, as a control signal for prosthetic hands, arms, and legs, and to remotely control computerized devices including flight systems, keyboards, and even interactive video games.

The physicians at Mountain Medical Practice are continually working to improve the quality of medical care provided to patients with muscle and nerve disorders.